“Rhinoplasty, skin grafts, and facial reconstructions have been practised for centuries. However, it was New Zealander Harold Delf Gillies who standardised these techniques and established the discipline of ‘plastic surgery’. In 1920, his text book “Plastic Surgery of the Face” was published, setting down the principles of modern plastic surgery; principles which were adopted by surgeons from every part of the world. The British Medical Journal described it as “one of the most notable contributions made to surgical literature in our day”.The New York Medical Journal said that “his are the greatest of all contributions to the advance of this interesting reparative work.”
The First World War was a challenge to most surgeons. The introduction of more destructive weapons resulted in devastating injuries. In addition, in trench warfare the head was more exposed than the rest of the body, and soldiers’ faces were often shattered or burnt beyond recognition. Despite the best efforts of surgeons, many soldiers were left hideously disfigured. A new type of surgery was needed. Realising this need a young surgeon operating out of Aldershot hospital, England, began performing operations which involved rebuilding the face by taking tissue from other parts of the body. This surgeon was Harold Delf Gillies; a New Zealander considered by many to be the father of plastic surgery.
Gillies was born in Dunedin, New Zealand, on the 17th of June 1882, the youngest of eight children to Robert and Emily Gillies. Although his father died when Harold was four, he did not leave his family destitute. He had been a successful land agent, a Member of Parliament, and a leading figure in Dunedin’s business community. In an unpublished memoir, Harold’s older brother wrote that “we were well endowed with the world’s goods through my father’s successful efforts”. These efforts made it possible for Harold to attend preparatory school in England, and later join his brothers at New Zealand’s Wanganui College.
Although little is known about Harold’s academic ability, it seems that he excelled at most sports, particularly cricket. While at Wanganui College he captained the First XI team in a series of matches, including one against Australia in 1900. That same year he was named best young player in the country. He entered Cambridge University (England) in 1901, and again it was his sporting prowess that marked him out. He became a first rate rower and was instrumental in helping his team win at Henley in 1902. He also represented his University at golf three times reaching the semi-finals of the Amateur Championships at St Andrews in 1903.
But Harold’s natural abilities were not confined to the sporting arena. He also proved to be a competent painter, a talent which first surfaced during his youth and culminated with an exhibition of his work in 1948 at Foyale’s Art Gallery, London.
It is probably no coincidence that Harold Gillies became outstanding in the practice of ‘aesthetic, reconstructive surgery’ (as he later described the field). While his physical dexterity made him a master surgeon, his artistic ability underpinned much of the work that he later did in reshaping people’s badly disfigured faces. A colleague of his once wrote that “in many hundreds of hours spent assisting or in watching Gillies in the operating room I never once saw him perform a hurried or rough movement. All the actions of his hands were consistently gentle, accurate and deft.”

Gillies’s family; Harold, the youngest, in white tunic (photo from: Gillies; Surgeon Extraordinary, Reginald Pound, 1964).
From Farm Boy to Surgeon Extraordinaire
Much of Harold’s youth was spent on the family farm. Gillies often reminisced about a happy childhood; a childhood “full of fishing and wild turkey hunting and of riding through rolling landscapes on the rump of the razor-backed family mare called Brogo”. He spent most of his school holidays with his brother Bob, who had a small farm in the South Island. During his stays he did sheep shearing jobs on neighbouring farms to earn money for university, and in his spare time he went fly fishing with his brother who was a keen angler.
Two of Harold’s brothers had already been to Cambridge University by the time he arrived there in 1901. The contrast between New Zealand and England could not have been more marked. Taking a coach from Southampton, he arrived at Caius College (Cambridge) which he later described as “a psychological and architectural blot”.

Gillies at Cambridge, 1902. Permission: Andrew Bamji, The Gillies Archives of Plastic Surgery.
“Abandon hope all ye who enter this bloody tunnel” he wrote – but his veneration for the College was never in doubt.
Despite his distaste for Cambridge, Gillies excelled both socially and academically. He became one of the most popular students at Cambridge and was well known for his practical jokes. On one occasion, a college head who was about to drive off in his Panhard found that the back axle had been jacked up. The joke had been masterminded by Gillies. Conversely, a fellow student by the name of K.D Pringle recalled that Gillies was a “versatile and brilliant man” who was entirely devoted to his studies. When others would meet after lectures for coffee and conversation, Gillies would go to his room and continue studying.
Gillies claimed not to know why he chose medicine as a career and when asked, he replied; “I think it was something to do with my having two brothers who were lawyers.” But given his physical dexterity, Gillies had a natural facility for surgery and this led to him undertaking formal training at St Bartholomews Hospital, London. He was appointed house surgeon to Douglas Harmer, head of the newly created Ear, Nose and Throat Department. Upon Gillies qualifying in 1910, Harmer wrote, somewhat prophetically; “I think there is every reason to believe that he will attain to a high position in his profession”. That same year Gillies was made a Fellow of the Royal College of Surgeons and awarded St Bartholomews’ Luther Holden Research Scholarship.

Gillies (top R) with fellow lodgers, Holland Park, 1907 (photo from: Gillies; Surgeon Extraordinary, Reginald Pound, 1964).
The Founder of British Plastic Surgery
Gillies was 32 when World War 1 broke out. Anticipating that he would soon be drafted, he joined the Red Cross and was subsequently sent to Belgium as a commissioned officer. On his way to Belgium, a series of chance happenings occurred which turned him away from general surgery and gave him an interest in ‘plastic work’. In the Channel port of Boulogne, he met Frenchman Auguste Valadier. Valadier who had set up a special medical unit for treating jaw wounds, was experimenting with taking tissue from other parts of the body – a process that greatly excited Gillies. He also met up with American dental surgeon Bob Roberts who lent him a German book on the topic of jaw and mouth surgery. Reminiscing about the incident, Gillies wrote: “I realised that I had struck a branch of surgery that was of intense interest to me,” and added, “My first inspiration [for plastic work] came from the few pictures in that German book.”
Buoyed by these events, Gillies went to Paris to seek a meeting with Europe’s foremost surgeon: Hippolyte Morestin. Morestin received him courteously and allowed him to watch an operation for cancer of the face. Gillies watched as Morestin removed the cancerous growth and then mended the wound by rolling up a flap of skin from under the patient’s jaw. Although this method was not new, it was a new experience for Gillies. After observing Morestin, Gillies wrote: “I felt a tremendous urge to do something other than the surgery of destruction”.
Gillies wasted no time in making a submission to the British Army for a plastic surgery unit. He undoubtedly felt a sense of urgency as the French had already set up plastic surgery units in Boulogne, Etaples, Amiens and Paris. As Gillies discovered, the French were not too keen on sharing their knowledge. On a second visit to Morestin, Gillies was refused entry to the operating theatre where previously he had been made welcome. An American who saw some of the work going on there told Gillies that much of it was crude.
On the 11th of January 1916, Gillies was ordered by the War Office to Cambridge Military Hospital, Aldershot, “for special duty in connection with Plastic Surgery”. His request for a British unit had been granted: he was to be Britain’s first plastic surgeon with full responsibility for getting the Aldershot unit up and running. Pragmatic as always, he spent £10 of his own money and bought labels directing all jaw and face injuries to himself – care of Aldershot hospital. He then went back to the War Office and handed them the labels, requesting that they be delivered to field hospitals in France. Within a few weeks wounded men began arriving at Aldershot with his labels pinned to their uniforms. Thanks to Gillies, plastic surgery in Britain was about to become a reality.
“A Strange New Art”
Rebuilding the face by taking tissue from other parts of the body was not a new idea. For centuries, Indian surgeons had been practising a form of rhinoplasty, where crescent shaped flaps of skin were drawn from patients’ foreheads and fashioned into substitute noses. During the 19th century, the French and Germans had developed a technique whereby skin could be transferred from one part of the body to another.

An Advanced Dressing Station in France, Henry Tonks (1918).
Indeed, by the time Gillies arrived on the scene, they had made considerable progress in plastic work “but appearance was of secondary importance”: “No one, it seemed, had given serious consideration to the aesthetic side, not even the French, who might be thought sensitive to it.”

Henry Tonks in his room at the Queen’s Hospital, (Royal College of Surgeons’ Photographic Unit).
For Gillies, plastic surgery not only involved restoring function but also making the person look normal and sometimes more beautiful than before. He was driven by the idea that the surgeon should be creative, imaginative – in fact an artist. He described his work at Aldershot as “a strange new art”, and indeed it was, for prior to Gillies there was little concern for how the patient looked. Gillies never wavered in his belief. Many years later, at the first International Congress of Plastic Surgery in Stockholm (1955), he declared; “within us all there is an overwhelming urge to change something ugly and useless into some other thing more beautiful and more functional.”
The art theme underpinned much of Gillies’ work. For example, in addition to describing his work in written form, he was the first surgeon to make pictorial records of pre- and post-facial reconstruction cases. Gillies initially undertook this task himself but the job was eventually given to a more accomplished artist, Henry Tonks. Tonks, a surgeon and also a teacher at the Slade School of Art, became the graphic historian of World War l injuries to the face and a noted wartime artist.

Plaster casts of faces of WWI patients, (photo from: Gillies; Surgeon Extraordinary, Reginald Pound, 1964.)
Sixty-nine of his pastel drawings, recording the scope of Gillies work, are in keeping at the Royal College of Surgeons, London (on permanent loan to the RADC Museum, Aldershot). Eighty-two paintings, all of which depict the horrendous injuries suffered by New Zealand servicemen, are at Queen Mary’s Hospital, Sidcup.
In addition to making pictorial records, Gillies spent at least an hour before each operation visualising the final outcome.He would pace up and down the hospital in aworld of his own, scribbling designs on pieces of paper, cutting them out with scissors, and then fitting them back together in a jigsaw-like fashion. He sometimes used a lump of wax in order to mould onto it the features an contours he hoped to restore to the patient’s face.
But his usual method was to create a plaster model of how he imagined the patient’s face would eventually look. Gillies was without a doubt the consummate surgeon-artist.
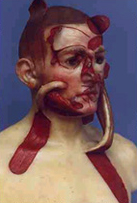
A life-size wax model illustrating surgical techniques Permission: Andrew Bamji, The Gillies Archives of Plastic Surgery.
The scope of Gillies’ artistry is captured in an operation that he performed on one J. Maggs, a Welsh Guard, whose nose had been completely severed by a sniper’s bullet. Using skin drawn from the forehead, Gillies made a replacement nose which was literally ‘perfect’. Indeed, it was so perfect that Gillies was forced to prove its authenticity. Thus, in 1918, J Maggs was exhibited at the British Medical Association’s annual meeting. At the end of the meeting Maggs was called to an ante-room where Gillies was waiting with a group of medical colleagues. As Maggs entered, he was greeted by Gillies in a foreign tongue. Not understanding, Maggs blushed. “Look, look,” exclaimed Gillies, pointing out that there was blood circulating to the nose and surrounding tissue.
Sir Charles Kenderdine, who helped Gillies establish a more advanced plastic surgery unit at Queen Mary’s Hospital (Sidcup), would show people three photographs of the same patient: one showing a shockingly disfigured face; the other showing the face after restoration; and a third showing what the patient looked like prior to disfigurement. His point in doing this was to show people that Gillies could actually make the patient look better than he had prior to disfigurement. “Don’t you agree?”, Sir Charles would say, “Gillies has actually improved his looks”.
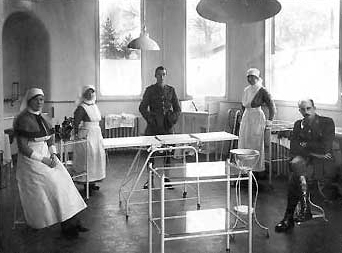
Plastic surgery theatre, Queen Mary Hospital, 1917. Gillies is seated on the right. Permission: Andrew Bamji, The Gillies Archives of Plastic Surgery.
The Innovator
Seeking to make the patient look better necessitated some major innovations; These were largely initiated by Gillies and which later became standard practice in plastic work. His most notable innovation, the pedicle tube, came about purely by chance. On October 3, 1917, an Able Seaman by the name of Vicarage was wheeled into the operating theatre at Queen Mary’s Hospital. All the skin had been burnt off his face in a cordite explosion on H.M.S. “Malaya.” The burns had left extensive scarring. The eyelids and lower lip were turned inside out, and all that remained was a twisted blob which had once been a nose. Gillies described the injuries as “appalling”. Cutting the skin off the patient’s chest, he made a scroll large enough to cover his face. Adequate blood supply was ensured by leaving the lower ends of the scroll attached to the chest. Apertures were then cut for the mouth and eyes and when it was stitched into position, it was given added blood supply from two thinner strips of skin raised from the shoulders with the free ends grafted on to the new face. While raising the skin from the patient’s shoulders Gillies noticed its tendency to curl inwards. Then came a flash of inspiration:
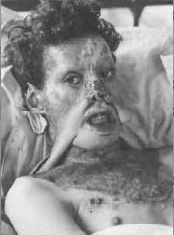
Seaman Vicarage and the worlds first pedicle tubes Permission: Andrew Bamji, The Gillies Archives of Plastic Surgery.
“If I stitched the edges of those flaps together, might I not create a tube of living tissue which would increase the blood supply to grafts, close them to infection, and be far less liable to contract or degenerate as the older methods were?” … “another needle was threaded and, in an astonished silence, I began to stitch the flaps into tubes”.
This innovation proved extremely successful and within a few weeks, tubes were seen sprouting from scores of his patients. The pedicle tube simplified grafting and made it more certain that a shattered face would be recognisable again. More importantly, the patient could return to society with some semblance of normalcy. Looking back, Gillies stated that it was “a major breakthrough, which I had good reason to be proud of.”
The horrific injuries suffered by Vicarage also led to another major innovation. While walking home late at night in the midst of an air raid, Gillies became deeply worried about his patient’s eyelids. The seaman could not close them and he was forced to sleep through the air raid with his eyes open. Reminiscing about the incident, Gillies wrote; “the idea suddenly came to me, a new way of restoring function and appearance to reverted eyelids”. The method that Gillies subsequently used on Vicarage became known as the ‘epithelial outlay technique!
“A considerable amount of doubting interest was aroused,” he wrote. “But when in two weeks the stitches were removed … there was shining before us the most perfect lid we had so far accomplished”.
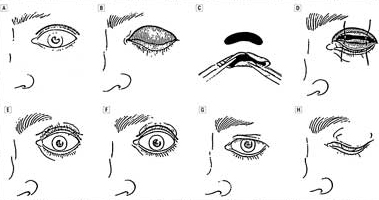
Stages in the epithelial outlay operation.
The ‘epithelial outlay technique’ and ‘pedicle tube’ were not his only innovations. Later in his career, Gillies used what he called an ‘intranasal skin graft’ to correct a nose defect caused by leprosy. This established a new principle in the treatment of facial disfigurement from leprosy. He also pioneered a new method for re-attaching severed limbs. This involved de-gloving the amputated section of skin and suturing the limb on bone to bone, tendon to tendon, and nerve to nerve. The technique proved successful and a similar method is still being used today.
It was Gillies too who was largely responsible for establishing a collaborative relationship between the general surgeon and the plastic surgeon. In the 1930s, a general surgeon by the name of Gordon-Taylor urgently requested Gillies help. His patient, a famous tennis player, had a number of malignant tumours and required surgery which involved removing his entire lower lip, part of his jaw, left check, and upper lip. Recalling the incident, Gillies wrote; “Gordon-Taylor had faith that a destruction could be reconstructed”. Indeed, Gillies was successful but it took four years of grafting to replace the lost tissue!
That was the first recorded instance of collaboration, which is now standard practice.
From Plastic to Cosmetic
Perhaps Gillies’ greatest innovation, if it can be called that, was the pioneering of what is known today as ‘cosmetic surgery’. After the war, Gillies continued to operate on ex-servicemen his roll of patients slowly diminished. To compensate, he established his own private clinic at 56 Queen Anne Street, London. The clinic was a huge success, not least because of his good reputation and a knighthood in 1930. However, it was not long before he was visited by clients of a different genre; clients who wanted to look better or more beautiful, despite having no apparent deformity.
During the 1930s, society women, film stars, and stage folk of both sexes came to Gillies for face lifts. “A golden haired star,” he recalled, “was so famous that everything had to go well.” His assistant of the time, cutting the sutures around the ear, accidentally snipped off the lobe. “The precious piece was sewn on again in double quick time without the patient being aware of it”. One of his face lift patients, a prominent London society woman, demanded a repetition of the operation every six months. “She looked marvellous for three weeks, then dropped back”, Gillies said. “When she began to look like a Chinese dance-hall hostess I decided that it was time to stop. She stalked off to spoil some other surgeon’s reputation”.
Face lifts were not the only cosmetic changes Gillies helped pioneer. He and his and cousin Archibald McIndoe, a fellow plastic surgeon and New Zealander, published a paper in 1938 on their mammaplasty technique devised for correcting breast abnormalities. In 1941, while on a lecture tour in the United States, Gillies told an audience at Galveston University, Texas how he once operated on the breasts of an amateur golfer: “once because they impeded her swing and the second time at her lover’s request.” While such operations were normally condemned by society and the medical fraternity, Gillies had an attitude that was ahead of his time: “From the psychological point of view the patient finds herself able to go among her friends with a new-found equanimity”. “Those girls … with a sensitiveness amounting to melancholia regain their self-confidence.”
Gillies was also ahead of his time in carrying out sex change operations. One such operation involved two sisters who were volunteer fire fighters. “Realising that they were more male than female,” Gillies wrote, “they came to consult me”. Their case was one of hypospadias, where “the forces which bring about ‘maleness’ or ‘femaleness’ have not yet exerted their influence on the genital organs.” After Gillies had operated on them, they were absorbed into society as ‘normal brothers’. In another case, endocrinologists and psychiatrists called on him to perform a sex change operation on a male patient who had a strong urge to be female. Because the operation became the subject of ethical protest and media sensationalism, the procedure undertaken by Gillies was never divulged. However, it is said that Gillies performed “a remarkably ingenious operation, believed to be the first of its kind”.
It is true that between the Wars Gillies increasingly dealt with cosmetic cases, but he always considered cosmetic surgery to be nothing more than a “subordinate extension of reconstructive surgery” the bulk of his patients were still people seeking relief from hideous injuries caused by accidents. A case in point was a Mrs Brown who, during an epileptic fit, had fallen into the red-hot embers of an open fire. Gillies described her as “a ghastly cinder of a woman”.:
“The coals had roasted her nose and lips completely away. Scarred opaque round objects once her eyes stared at me. What a harrowing decision confronted me! She sat there quietly while I studied her, weighing up in my mind if it were justifiable to accept the challenge to try to make her a new face. In spite of all this, the decision to operate came quickly.”


Knowing that total success was beyond their reach, Gillies and colleague Pomfret Kilner rebuilt Mrs Brown’s nose and cheeks. Her exposed sinuses were clothed again, her eyebrows renewed, and her mouth given new lips. They even hoped that her sight might be restored and called in an ophthalmic specialist – but to no avail. Feeling that the best tonic for Mrs Brown would be the heartfelt approval of her family, Gillies sent her to Elizabeth Arden’s salon in Bond Street where she was given the most expensive cosmetic treatments available. Sadly, some months later, Gillies received news that Mrs Brown had died during one of her fits. “Poor Mrs Brown,” Gillies was heard to murmur with his head bowed in grief.
Another patient, Jean Dawnay (later to be Princess George Galitzine) had, as a 4-year old, the upper half of her face coated with boiling tar and bitumen in a road-side accident. Fearing permanent damage to the exposed wound Jean was taken for treatment to Gillies’ practice.
The operation was a complete success, featured in Lancet, and, in an outcome redolent of a Hollywood melodrama, Jean would go on to become a leading model for Christian Dior and Jacques Fath and marry a Russian prince. “Nothing would have happened you see”, she recollects, “without Gillies and McIndoe”.
The Father of 20th Century Plastic Surgery
Between the Wars, the name Harold Delf Gillies became synonymous with plastic surgery. Gillies was undoubtedly the founding father of this newly established discipline and there was no greater evidence of this than in the United States. Following a lecture tour there, Gillies noted the “springing up of a large group of USA plastic surgeons”. Many of them had seen Gillies operating during the war, and many more had been tutored by him after the war. His popularity was so great that in 1941 when he was guest of honour at the American Congress of Ear, Nose and Throat (Chicago), more than 2000 came to hear him speak. At the age of 78, he was given the Special Honorary Citation of the American Society of Plastic and Reconstructive Surgery, in recognition of his “development of the speciality of plastic surgery,” and his “outstanding scientific contributions to the advancement of its practice.” Today Gillies is remembered each year when the American Academy of Facial Plastic and Reconstructive Surgery gives out its Harold Delf Gillies Award for best science research paper.

Gillies tutoring students in Austria, 1954.
In addition to Americans, Gillies had trained literally hundreds of surgeons from the ‘dominions’. At Queen Mary’s Hospital in the 30s there were teams of surgeons from Canada, Australia, and New Zealand. and many of them became founders of plastic surgery in their own countries. One such surgeon was fellow New Zealander Archibald McIndoe who arrived in Britain via the United States. When Gillies took him under his wing in 1930, he would not have known that some of McIndoe’s feats would one day be as great as his own.
Scores of surgeons from these countries were also trained by Gillies after the war.
The Return Home
Harold Delf Gillies died in July 1960 but not before returning to his native New Zealand. Homesick after nearly 51 years absence, he flew off with his wife in the late autumn of 1955. Prior to leaving England, he told a close friend that:
“I want to smell the New Zealand bush on a wet day, I want to hear the tui, catch a brown trout, do a little painting, and perhaps play three or four holes of golf. And I want to see the pohutukawas in full bloom”.

The Tui – notable mimic
While in New Zealand he addressed a meeting of the Royal Australasian College of Surgeons in Christchurch, and visited his son, John, who was living near Dunedin. Such was his ‘mana’, that the New Zealand Government gave him free local transport, free railway travel, and free accommodation. In Wellington, he was guest of honour at a special banquet given by Prime Minister Sidney Holland.
A Final Tribute
In 1962, the distinguished British surgeon Sir Heneage Ogilvie wrote that “during my life I have only known three surgeons who were undoubtedly first-class. They were Geoffery Jeferson, Harold Gillies and Russell Brock. Apart from Arbuthnot Lane, who was before my time, they are the only men in Europe or America who have taken a branch of surgery and by their own effort, by their leadership, their research and craftsmanship, have left it far higher than they found it. To say that of Gillies is an understatement: he invented plastic surgery. There was no plastic surgery before he came. Everything since then, no matter whose name be attached to it, was started by Gillies, perfected by him and handed on by him to lesser men, who have often claimed it as their own.”

REFERENCES AND BIBLIOGRAPHY
Books and Written References:
Bank of New Zealand, Wellington (1967). Notable Scientists. Martin printing, Napier
Grayland, Eugene (1968). Famous New Zealanders; Whitcombe and Tombs, New Zealand.
Pound, Reginald (1964). Gillies; Surgeon Extraordinary. Michael Joseph Ltd, London. Whitcombe & Tombs, New Zealand.
Internet References:
[All pages accessed June 2002]
Bamji, Andrew. Dr (2002). Queen Mary’s Hospital Sidcup, UK: The Gillies Archives of Plastic Surgery. An archival resource, much of which is reproduced online, including the “not-for-the-squeamish” Macalister Watercolours collection of injuries suffered by New Zealand soldiers at Queen Mary’s Hospital. http://website.lineone.net/~andrewbamji/index.htm
Douglas, L.G. Dr (1997). Canadian Society of Plastic Surgeons – ‘Tribute to our founders’. The Canadian Journal of Plastic Surgery, 1997, Volume 5, Number 1. http://www.pulsus.com/Plastics/05_01/foun_ed.htm
Gilman, Sander. L (1999). Making the Body Beautiful: A Cultural History of Aesthetic Surgery. Princeton University Press. Reproduction from the first chapter of Gilman’s book tracing the cultural history of the discipline.
http://pup.princeton.edu/chapters/s6545.html
Triana, Rudy. J. MD (1999). Sir Harold Gillies. Archives of Facial Plastic Surgery, Vo1, No 2; April-June 1999. http://archfaci.ama-assn.org/issues/v1n2/ffull/
qps81000.htm
Further web pages of interest:
Illman, John (2002). ‘Transsexuals – Born In the Wrong Body’, in Channel Four Health. An Article featuring Gillies as a pioneer of sex-change surgery.
http://www.channel4.com/health/microsites/H/health/magazine/sexchange.html
Parker, Stephen, (2002) ‘Harold Gillies 1882-1960.’ A brief bio of Gillies, in surgical-tutor.org.uk:
http://www.surgical-tutor.org.uk/default-home.htm?surgeons/gillies.htm~right
Biographical page on Ralph Millard, considered one of the “10 greatest American plastic surgeons of the millennium” … and trained by Gillies
http://calder.med.miami.edu/Ralph_Millard/biography.html
The Facemaker – Stuart Hoar play about Gillies’s Kiwi cousin, Alexander McIndoe, also a famous plastic surgeon.
http://www.courttheatre.org.nz/index.cfm/4,259,35,49,html

Prior, Rupert, (winter 2001) ‘Princess George, model patient’, in The Blond McIndoe. An article on Gillies’s famous reconstructive efforts on Jean Dawnay:
http://www.blondmcindoe.demon.co.uk/bulletins/pdfs/winter2001.pdf
[No longer active October 2006]
American Academy of Facial Plastic and Reconstructive Surgery. An article tracing the history of the academy that details Gilies formative influence and the award named in his honour:
http://www.facemd.org/patient/about_us/h_war.html
Story by CJ Williams, June 2002.
CJ Williams is a BA, BSc (Hon) and MSc graduate of Victoria University, with majors in history, sociology and psychology. He is a social and behavioural scientise, multi-media producer and writer of various forms. His main area of interest is the interplay between free choice, fate, individual behaviour and social environment.













Back in civilian life...Dame Cecily Pickerill pioneer plastic surgeon. She was trained by her l(ater) husband and repaired so many NZ children. This by using mother’s to care for their own babies. Infection was prevented completely by having mother and baby insulated to their own room or outside in the fresh air. Mothers mixed with each other everywhere except in the bedroom...insulation not isolation.! This before there was any training for plastics being offered as a training by Gillies in 1945. Her country NZ saw Dr Cecily for what she was doing and made her our first medical Dame. See ...A Dame we Knew, By Beryl. Harris.
"Your list of New Zealand heroes is impressive, and I would like to add three more names; Harold Gillies',CBE, FRCS (1882-1960), Archibald McIndoe M.B, ChB, F.R.C.S (1900-1960), and William Alban Phillips, PhD (1914-1975). These are three New Zealanders that have left their marks on the world. Gillies for example is considered the founding father of modern plastic surgery. Although his specialty was facial plastic and reconstructive surgery, Gillies' interests included microvascular surgery, and the reattachment of amputated limbs. His maxim of "never throw away anything until you are sure you do not require it" is followed in all fields of plastic surgery to this day. McIndoe was the cousin of Harold Gillies and was also a pioneering plastic surgeon who worked primarily with WWII burns victims, particularly fighter pilots. It was McIndoe who made the connection between the recovery rate of burns victims who had fallen into the sea and the concept of saline baths for burns victims. Prior to that an oil solution was used on their burns. Finally, William Alban Phillips' area of expertise was economics. He is best known for his infamous 'Phillips Curve' which models a trade-off between inflation and unemployment. You will not find any modern economic text that does not have a section on the Phillips Curve. Needless to say, Phillip's model has influenced the economic policy of countless governments throughout the world, yet few New Zealanders have ever heard of him." Craig Wellington, New Zealand